Transforming care for the 30 million newborns who require medical care, and who are currently being left behind, is a smart investment in the health and development of future generations. Kangaroo Mother Care (KMC) is one of the leading proven interventions that can radically improve inpatient care for small and sick newborns, leading to shorter hospitalizations and improved health outcomes.
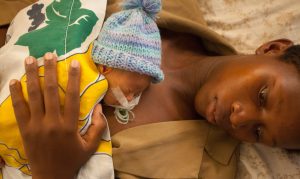
KMC refers to the practice of providing early, continuous, prolonged skin-to-skin contact between mother and baby, exclusive breastmilk feeding, and follow-up care with high-risk newborns. It has shown to decrease mortality and morbidity in preterm and low birthweight infants by providing protection from infection; regulating temperature, breathing, and brain activity; and encouraging mother-baby bonding. In many cases, newborns who receive KMC are able to be discharged early from the hospital and KMC can be continued at home. When delivered as a complete package, it is highly effective at reducing newborn mortality – up to 40% according to recent data.
14.7
percent of infants with low birthweight globally (2020)
27
percent of infants who were not weighed at birth globally (2014-2020)
40
percentage reduction in mortality of low birthweight infants (<2000g) who receive KMC compared to conventional neonatal care*
All data on this page represents the most recent data available, unless otherwise noted. Please visit our Newborn Numbers page and download the Excel spreadsheet to explore the data further.
KMC implementation

The World Health Organization (WHO) recommends KMC for the routine care of newborns weighing 2000 grams or less at birth, regardless of availability of incubator care. Recent studies are showing a significant decrease (25%) in morbidity and mortality for newborns who begin KMC immediately after birth, especially in newborns weighing between 1 kg and 1.79 kg. KMC can and should be started as soon as possible following birth, and can occur while stabilizing care is provided to the mother and newborn (eg, newborn receiving continuous positive airway pressure (CPAP) for respiratory distress). Additionally, recent studies have shown that KMC can be effectively implemented at home for newborns who are born outside of a facility, although all small newborns should receive post-natal care and follow-up with health care providers.
There is a global push advocating for skin-to-skin contact between mother and newborn for one hour immediately following birth for all newborns, regardless of size at birth. While skin-to-skin contact is a key component of KMC, skin-to-skin alone is not sufficient for small newborns. All small newborns should receive complete KMC care, depending on facility and national protocols.
KMC is considered a part of family-centered, respectful newborn and maternal care. It can be implemented during the full continuum of care, and is especially effective transitioning from the facility to the household. Providers should be trained to educate mothers and fathers in home-based continued KMC, and encourage its use at the home following discharge. Additionally, early and immediate KMC can also support positive early development, beyond the physical health benefits and morbidity prevention.
Accelerating KMC uptake

Despite the many benefits of KMC, country-level adoption and implementation have been limited, and only a small proportion of newborns who could benefit from KMC receive it. Barriers to KMC implementation at the facility level include inadequate facilities and supplies for KMC, insufficient staffing in facilities, lack of training and prioritization of KMC by facility staff, and inadequate policy and professional commitment to KMC. At the family and community level, barriers include cultural norms that make practice of skin-to-skin care difficult, lack of family and financial support for mothers to practice KMC, limited understanding of KMC, and stressors related to extended hospitalization.
The COVID-19 pandemic was and continues to be a barrier for implementation of KMC in most settings. Infection prevention measures during the pandemic led to more newborns being separated from their mothers immediately following birth, even low birthweight and preterm newborns who would benefit from KMC. It is critical that infection prevention policies and government agencies do not recommend separation of mother and newborn, so that all vulnerable newborns receive KMC, even during COVID-19 outbreaks and infections.
Key resources
Guidance
- Global Position Paper on Kangaroo Mother Care: A transformative innovation in healthcare (2023)
- Kangaroo Mother Care: Implementation strategy for scale-up adaptable to different country contexts (2023)
- WHO recommendations for care of the preterm or low-birth-weight infant (2022)
- Standards for improving the quality of care for small and sick newborns in health facilities (2020)
- Survive and Thrive: Transforming care for every small and sick newborn (2018)
- Joint Statement: International WHO Recommendations on Interventions to Improve Preterm Birth Outcomes (2017)
- Kangaroo Mother Care Joint Statement (2016)
- Kangaroo Mother Care challenge brief (2016)
- Kangaroo Mother Care Implementation Guide (2012)
Research
- Effect on neonatal sepsis following immediate kangaroo mother care in a newborn intensive care unit: a post-hoc analysis of a multicentre, open-label, randomised controlled trial (2023)
- Barriers and facilitators of facility-based kangaroo mother care in sub-Saharan Africa: a systematic review (2021)
- Immediate “Kangaroo Mother Care” and Survival of Infants with Low Birth Weight (2021)
- Effect of community-initiated kangaroo mother care on survival of infants with low birthweight: a randomised controlled trial (2019)
- Kangaroo mother care: a systematic review of barriers and enablers (2015)
Country Specific Resources