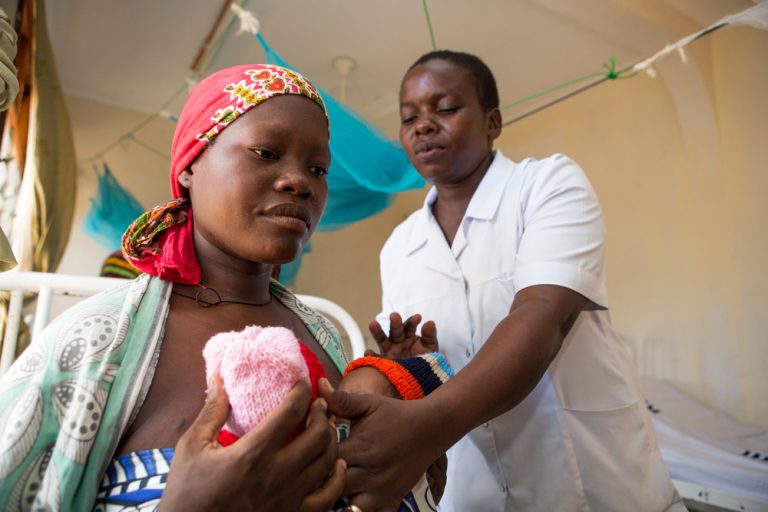
A recent study on the measurement of service readiness for providing inpatient care of small and sick newborns puts the spotlight on improving monitoring systems, quality of care and investments in health systems scale-up to end preventable newborn death and disability, as discussed in Part 2 in a series of three online thematic discussions surrounding newborn care, hosted by CHIFA. Please see the discussion’s introduction article for more information.
Part 1 of this global conversation sought to understand the situation regarding newborn care worldwide and the many gaps and issues; see the HNN blog here (see also Full Text, Long Edit and Short Edit versions).
Part 2 of the discussions looked at the health system and the actual implementation of quality care for small and sick newborns – who is caring for the newborn and where, is care ‘family-centred’, what infrastructure do we need, who are the key players in global newborn care, how can we ensure accountability and measure care within all levels of the health system? See here for the full text, long edit and short edit versions.
From 19 February to 30 March 2018, Part 2 of our online discussion involved 99 contributions from 40 CHIFA members in 18 countries (Brazil, Canada, Georgia, India, Kenya, Nigeria, Pakistan, Philippines, Rwanda, South Africa, South Sudan, Sudan, Sweden, Tanzania, Turkey, Uganda, UK, USA). As before, this discussion was structured around specific questions, and is summarised below.
1. Who is the health worker caring for the newborn? In your countries and programmes who is caring for small and sick newborns? Midwives and nurses? Who are the champions of newborn care?
CHIFA members described the healthcare providers caring for the newborns in the community as including: traditional herbalists/native doctors, religious leaders, traditional birth attendants, community health workers and community midwives/nurses with community health workers mentioned most frequently. Development of information systems and efficient referral links were described as especially important for connecting care in the community with facilities.
Regarding staffing for inpatient care of small and sick newborns, there was a passionate response from CHIFA members regarding the inadequate numbers of staff, especially nurses (up to 30 babies per nurse at night), with their ability to implement quality care further hampered by working long hours with low pay, minimal training, supervision and support, along with inadequate resources. CHIFA members gave examples of how this has been tackled, including protection against rotation, advocacy for specialised neonatal nurse training, monthly outreach support visits to level 1 hospitals by paediatricians, and standardised clinical records and systems.
In the experience of many contributors, external or international “expert” healthcare professionals for newborn care were only found to be useful to local health workers and implementers when they aligned their guidance to the local policy context.
2. Where in the hospital are small and sick newborns cared for? What infrastructure, equipment, commodities, guidelines are needed for small and sick newborn care?
CHIFA members noted that district hospitals often do not have a neonatal unit or a space or specific ward. Small and sick babies are, therefore, often cared for on maternity units or postnatal wards. In tertiary hospitals where there are more often nurses that have received child/ neonatal nurse training, and access to paediatric trained doctors.
UNICEF recently published a report referring to 10 life-saving articles for newborn care: bag and masks, antibiotics, blankets/ cloths, chlorhexidine, CPAP machines, oxygen concentrators, phototherapy, micronutrient supplements (antenatal), tetanus immunisations, and thermometers. Some contributors found that oxygen was often in limited supply, necessitating sharing between babies, risking hypoxia/ hyperoxia and infection. Some CHIFA members noted that abreast pump was also deemed to be an important piece of equipment, to help mothers struggling with breastfeeding particularly those with preterm babies.
The availability and usage of updated standardised guidelines on empirical treatment is varied. The PACK Global programme by the BMJ is designed to comprise protocols that can be adapted to different contexts; we heard accounts of its successful implementation in Nigeria.
3. How is the family involved in caring for small and sick newborns? Are your facilities implementing kangaroo mother care? What does family-centred care mean in your context? What can be done to strengthen the quality of family-centred care?
CHIFA members reported wide variety in the extent to which the family is actively involved in care of small and sick newborns. In many settings, mothers are encouraged to carry out feeds and cares, support each other with KMC, and be present for ward rounds. Some settings support mothers in practising more medicalised tasks such as administering oral medications, giving NG feeds (in Rwanda one survey showed that 83% of units allow this), and checking temperatures. Numerous studies, including recent work in India, found that when implemented well family-centred care built the confidence and competence of the family to provide care after discharge. CHIFA members stressed the importance of safety and provision for families, including lodging facilities, parental literacy, and staff time to train parents. In Malawi, Every Preemie- SCALE is testing a family-led model of care involving guidance for healthcare workers on providing and monitoring KMC, low-literacy materials for the family, and referral links for community follow up; materials can be found at www.everypreemie.org.
Regarding Kangaroo Mother Care, there is widespread appreciation of the evidence for improved outcomes and the importance of the intervention; however many CHIFA members described implementation challenges including lack of resources (beds/ space, monitoring devices), lack of a ‘champion’ to drive this intervention, inadequate education/ incorporation into the training curriculum. Most contributors felt that these systems barriers were far more prevalent than a lack of willingness from mothers and families. Save the Children has been promoting the KMC Challenge since 2016 to raise awareness and open up dialogue around the enablers and barriers.
4. Who in the ministry is responsible for newborn programmes, at the national level? What about referral systems? What about measurement and accountability?
In many countries the Department of Health oversees comprehensive frameworks for maternal, newborn and child health, within which programmes for care of the small and sick newborn/ facility-based care are located and then implemented by coordinators at the district level. Despite encouraging policies, in many countries there is still a wide gap at the implementation level. CHIFA members gave encouraging examples of implementation process in India where in the last decade, this progress has included through the standardisation of operational & training guidelines, infrastructural revisions to promote family-centred care and KMC, launch of a breastfeeding program, creating mother-child tracking systems, and a uniform government online database that helps to monitor, audit & compare performances of neonatal units, with regular perinatal death audits and reviews.
In some countries the government provides national norms for resource requirements for neonatal units, and have standardised guidelines, medical and nursing records, and information systems, contributors described this as helpful for district coordinators. Clinical audit systems where seen as important when they were of high quality and linked to action.
5. Who are the key players in the global health architecture for newborn care? UNICEF is making newborns their advocacy priority this year. Is this the UN responsibility alone? What about WHO, donors, professional groups and academics?
A list created by CHIFA members includes: 1. World Health Organization 2. UNICEF 3. Partnership for Maternal, Newborn and Child Health 4. Save the Children International 5. Healthy Newborn Network 6. US Agency for International Development 7. Bill & Melinda Gates Foundation 8. International Confederation of Midwives 9. International Paediatric Association 10. International Federation of Gynaecology and Obstetrics 11. International Council of Nurses 12. American Academy of Paediatrics 13. Laerdal Global Health 14. LDS Charities 15. American College of Nurse Midwives 16. Council of International Neonatal Nurses.
Last month, UNICEF launched a campaign ‘Every Child Alive: the Urgent Need to End Newborn Deaths.’ It refers to the 4 P’s to enhance quality of care; Place (clean functional health facilities with water, soap and electricity), People (adequate number and training), Products (10 life-saving commodities/equipment), and Power (empowering girls, mothers and families to demand quality care).
The WHO Commission Report on Social Determinants of Health provides essential and convincing evidence for advocacy. Improvements in service delivery may have some impact but are not able to address the fundamental drivers of adverse perinatal outcomes; health professionals have a duty to address these drivers as well as promoting service improvements.
The Every Newborn Action Plan (ENAP) is a great step forward for newborn health collaboration and collective action, launched in 2014 and steered by many of the above listed actors, with a vision of a world “in which there are no preventable newborn deaths or stillbirths. where every pregnancy is wanted, every birth celebrated, and women, babies and children survive, thrive and reach their full potential.”
The third in this series of thematic discussions will start soon (date to be confirmed) and we invite you to join us at CHIFA today in readiness to share your valuable opinions and experiences.