The hallways are lined with women in labor. The beds are filled with mothers holding small or sick newborns. And the walls are plastered with various medical guidelines. This is the labor and maternity ward at Ntchisi District Hospital – one of four district hospitals participating in the quality improvement (QI) process for Malawi’s newborn health services. Led by the Ministry of Health with support from partners including Save the Children, the initiative aims to improve the quality of care provided to newborns and to create an institutionalized mechanism for shared learning across health facilities.
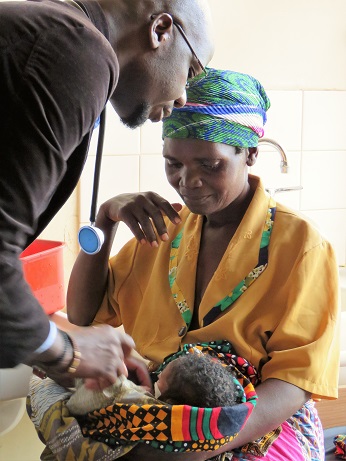
The road toward quality improvement in Ntchisi hasn’t been an easy one. It has been filled with roadblocks and unexpected obstacles as the staff and district health management team learn to navigate the challenges of providing quality care to newborns in a country where resources – human, infrastructure, and equipment – are inadequate.
When the QI program was introduced in Ntchisi, maternal and newborn health indicators were devastating – 16 neonatal deaths per 1000 live births and 88 maternal deaths per 100,000 deliveries[1]. Clinicians and nurses were rotated through the various departments disrupting the continuity of care. Documentation of newborns was almost nonexistent, meaning many births were uncounted. With limited record keeping and an absence of staff specially trained in newborn care, the monitoring and treatment of newborns was erratic, leading to many preventable deaths from treatable conditions. In short, babies were undervalued. This was the reality not only in Ntchisi but in district hospitals across Malawi, where newborn health lags behind that of progress made in maternal and under-five health. Today, newborn deaths still account for 42 percent of all under-five deaths in Malawi.
The QI initiative is addressing some of these challenges through mentorship, refurbishment, quality-of-care audits, and partnerships/collaboration. Ntchisi District Hospital has benefited from the structured mentorship program run by nurses and clinicians from Malawi’s central hospitals including Kamuzu Central Hospital (KCH) and Queen Elizabeth Central Hospital (QECH). The program sends selected district staff to a two-week clinical attachment at these central hospitals for intensive on-the-job training.

Through this attachment, onsite mentorship, and other specialized training, the hospital staff become better equipped to care for premature and low-birthweight babies, including supporting mothers to provide kangaroo mother care. It has also built their capacity to manage common complications of preterm birth, including treatment of postpartum hemorrhage, asphyxia, and sepsis.
“With the help of the mentors, the quality of care we give to the neonates has really improved and continues to move in the right direction,” said Solomon Mbewe, a Clinical Officer at Ntchisi District Hospital who participated in the mentorship attachment. Mbewe added, “There are things we take for granted and think we are doing well. But when you go to the central hospital for the attachment you are oriented to a different way of providing care. I can say that for me it transformed my conduct, my practice and my attitude. It is really powerful.”
In addition to building the skills of health providers, national mentors conduct regular supervision to provide feedback on the quality of care, including general environment/hygiene, organization of materials, and other areas. During a recent visit Dr. Ulemu Chikhadzula, a pediatrician and national mentor from KCH, noted “The conditions have changed a lot. When I visited last time, I didn’t find any clinician working on the babies. This time, I found a clinician who had been mentored now working in the nursery. I found dedicated nurses who had made a total care plan, and the environment was much cleaner in general. I can see that the clinicians and nurses are beginning to see the importance of taking care of the neonates.”
Other partners have supported the QI initiative by equipping the neonatal unit with basic equipment and supplies including a radiant warmer, continuous positive airway pressure (CPAP) machines, and mattresses for the wooden newborn cots.
Despite the progress made so far, the work must continue. With continued high rates of asphyxia, poor documentation, and congested space available for the neonates, neonatal deaths rates remain staggering.
“Most of the time the babies are still not counted, particularly in the post-natal ward where they may get sick but haven’t been tracked,” said Dr. Chikhadzula. “I feel that this shows that people don’t really value the neonates. Their value just isn’t recognized and it’s not a good thing, because we can end up losing a child while it is in the hospital or a baby can become very sick.”
As donor-funded projects phase out, the government’s continued commitment to newborn care becomes even more critical. “These programs need to continue because it is still just at the grassroots and really starting to show progress. It is very important and can make a big difference in saving the lives of our neonates,” Dr. Chikhadzula said.
This QI initiative has shown that reducing newborn mortality and improving the quality of care in Malawi is possible. But it remains an ongoing – and urgent – process.
The journey will continue to present obstacles, but with the commitment of clinicians like Solomon Mbewe and advocates within the Ministry of Health, the future for Ntchisi district hospital – and all of Malawi’s newborns – is bright.
[1] DHIS 2 QI 2016.
