Blog adapted from a comment in The Lancet Global Health here
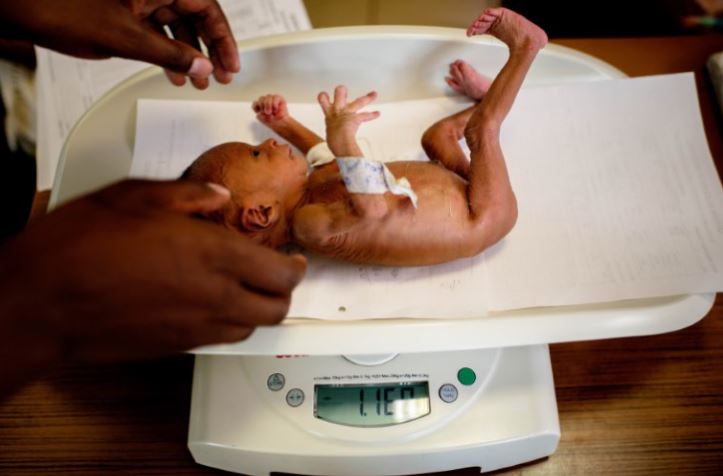
Birth weight is an important gauge of maternal and fetal health as well as an important determinant of perinatal, neonatal and postneonatal outcomes. Approximately 80% of newborns who die every year are low birth weight (LBW), under 2500 g, because they were either born preterm or small for gestational age or both. LBW newborns who survive have a greater risk of both short and long term adverse health consequences.
In 2012, countries committed to a 30% reduction of LBW by 2025 as one of the Global Nutrition targets. Monitoring trends within and across countries is necessary to track progress and crucial to achieving the Sustainable Development Goal for health. UN agencies have previously tracked LBW estimates using non-comparable, national data sources making it difficult to interpret and respond to patterns.
The new paper by Blencowe and colleagues presents the first systematic estimates of global, regional and national LBW trends incorporating new data sources and analytical approaches to adjust survey data for heaping, and missing data. The authors collated data from national administrative sources and nationally representative surveys for 148 countries of 195 UN member states. They estimated a worldwide LBW rate in 2015 of 14.6% resulting in 20.5 million LBW livebirths, with 91% from low-and-middle income countries. The global trend estimate presented shows an average annual rate of reduction in LBW of only 1.2% between 2000 and 2015, well short of the estimated 2.7% required to meet the target.
Their work brings to light the enormous inequities in data availability. Nearly half of all data points (48%) were from high-income countries. Only 13% of input data came from sub-Saharan Africa and Southern Asia, the regions with the highest LBW rates. National administrative data came predominantly from high (65%) or upper-middle income (28%) settings whilst for low and lower-middle income settings, the majority (54%) of LBW data points were from household surveys. Furthermore, 47 countries had insufficient data to generate a national estimate, 62% of these being low and lower-middle income countries.
Data on LBW prevalence is needed to assist countries in developing action plans and accountability measures and to monitor progress; yet many barriers prevent accurate LBW measurement. It is estimated that globally the birthweight of 48% of infants is not recorded, either because they are born outside of health facilities, or in ill-equipped health facilities, or due to weak health information systems. Routine administrative data sources, such as the District Health Information System 2 and civil registration and vital statistics (CRVS) systems, should be capturing data on birthweight. Investments in strengthening these routine data systems could enable greater local and national use of data for action and provide disaggregated information. In settings where routine information systems remain weak, surveys remain an important source for LBW data; and this paper has shown that analytical methods can be employed to adjust for methodological biases.
The authors present an urgent and practical call to action to greatly improve the coverage of weighing at birth including the need to count and weigh all babies (livebirths and stillbirths), strengthen existing data and health systems and innovate better weighing devices. Yet achieving this practically, especially in emergency settings or weak health systems, remains a challenge. While the paper calls for accurate gestational age measurement, which is a desperately needed component of high-quality antenatal care, birth weight remains a highly important and relevant indicator since accurate gestational age measurement is unlikely to be undertaken systematically in the immediate future in many settings where the burden is greatest.
Alongside improving measurement, multi-dimensional, context-specific national action plans are needed to achieve the Global Nutrition targets with support from funders and implementation partners. These should include improving nutritional status of women and girls, before and during pregnancy; treating pregnancy associated conditions such as pre- eclampsia and providing quality antenatal care. Furthermore, feasible, cost-effective interventions exist to reduce adverse outcomes amongst LBW newborns, such as Kangaroo Mother Care and household interventions such as early stimulation. Strong community-facility linkages are also required to identify and refer pregnant women at high risk of a LBW newborn or to address behavioural and social norms that negatively affect the care and survival of these babies. Digital health approaches, such as MomConnect in South Africa, also show promise.
With continued momentum on child survival and health, including early childhood development, these new LBW estimates provide an opportunity to advance the agenda and call upon all stakeholders to take concerted action in the effort to ensure that every newborn is weighed at birth, and that the information is collated and used for local action and accountability at the household, community, district, national and global levels. At the same time, we must improve care for the 20.5 million LBW infants and their families each year.