A blog by Steve Wall, Senior Advisor, Newborn Health at Save the Children
KMC Works, but Timing Matters
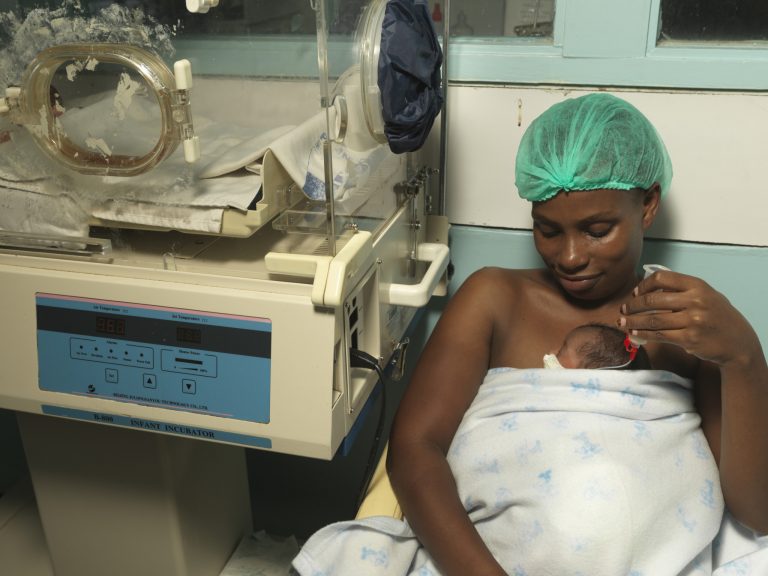
Kangaroo Mother Care (KMC) is one of the mainstays in our arsenal to save the lives of small babies. The KMC approach has been used across the world since first used and reported by Dr. Edgar Rey in 1983* as a life-saving remedy for fragile small babies in overcrowded nurseries in Colombia. With an expanding body of KMC evidence over the past two decades, the World Health Organization (WHO) currently recommends continuous KMC for stabilized newborns <2kg, and where KMC cannot be provided continuously, the recommendation is to provide intermittent KMC as much as possible. KMC has been shown to reduce newborn mortality by around 40%. But with KMC initiated after the baby has been stabilized, many or most deaths in small babies occurred prior to stabilization.** Several small studies posited that KMC, initiated immediately after birth or in the first hour, could potentially reduce the time to stabilization. These findings, re-examined more recently, suggested the potential benefits of immediate or early KMC initiated prior to stabilization, compared to the usual approach of KMC initiation after stabilization, most often in a KMC ward.
Summary of the WHO Study
WHO led a multi-center study of immediate/early KMC to test both the safety and efficacy of this approach. The results of this first-of-its kind study were recently published in the New England Journal of Medicine, and opened the door to a potentially powerful implementation approach for KMC to save the lives of thousands of small babies.
The study enrolled 3,211 newborns between 1kg and 1.79kg and their mothers from 2017–2021. The median duration of skin-to-skin contact in the neonatal intensive care units (NICUs) was 16.9 hours in the intervention group and 1.5 hour in the control group. Outcomes were neonatal death at 28 days and neonatal death at 72 hours. The main findings were a 25% reduction of mortality at 28 days in the immediate KMC group compared to usual care of KMC after stabilization (95% CI:36%, 11%). For deaths up to 72 hours, the effect was 33% reduction but with wide confidence intervals. The study found notable reduction in suspected sepsis and hypothermia in the intervention group, but there were no differences between groups in exclusive breastfeeding at the end of the neonatal period nor in full breastfeeding (by suckling) at hospital discharge.
Study Impact
The findings of this study can and should bring transformational changes in the care provided to small babies and their mothers/families. Already we are seeing major shifts in global and country policies. The concept of “zero separation” is one of the latest developments taking hold in the maternal and newborn health (MNH) movement. Humans are one the few mammalian species that routinely separate mothers from their newborns and young. The time for this transformation is past due, but now – for the first time – it is supported by new robust evidence. Over the last decade, we have seen nurturing care emerge as a key approach to infant and child growth and development. The WHO’s nurturing care framework applies across the spectrum of child and family care, and for small and sick newborns this care is seen as vital to survival and development to achieve the highest human potential. Models of family-centered care for small and sick newborns are becoming the norm in low and middle-income countries (LMICs) as well as in better-resourced settings.
Call to Action
The WHO study highlights the emerging need for government leadership in ensuring the structure, space, and design layout of Mother NICUs. Following the example of this study, Mother NICUs should be designed to provide adequate space and furniture with beds, comfortable chairs, and other amenities to make mothers as comfortable as possible. We also know that successful transition to home from hospitals includes continuation of KMC at home, especially for the smaller, more vulnerable newborns. Moreover, we now know that implementation of immediate KMC has the potential to save 150,000 newborn lives each year. It goes without saying that governments and donors should prioritize funding for this intervention, and stakeholders including professional bodies, implementing partners, and parent groups should clearly place these changes at the centerpiece of their future MNH advocacy and leadership.
* Rey E, Martínez H. Manejo racional del niño prematuro. Bogotá, Colombia: Universidad Nacional, Curso de Medicina Fetal, 1983
** Bergman NJ, Linley LL, Fawcus SR. Randomized controlled trial of skin-to-skin contact from birth versus conventional incubator for physiological stabilization in 1200- to 2199-gram newborns. Acta Paediatr 2004; 93: 779-85.
Chi Luong K, Long Nguyen T, Huynh Thi DH, Carrara HPO, Bergman NJ. Newly born low birthweight infants stabilise better in skin-to-skin contact than when separated from their mothers: a randomised controlled trial. Acta Paediatr 2016; 105: 381-90.