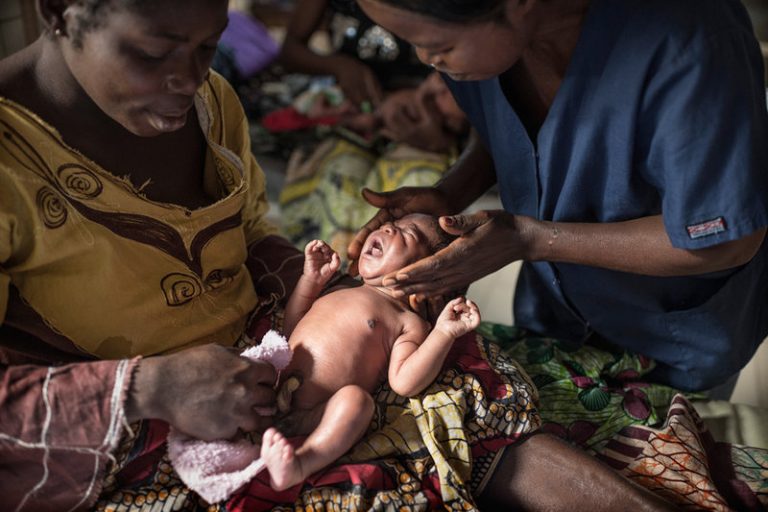
Enhancing health outcomes for pregnant women and newborns in developing countries has been a key policymaking goal over the last 20 years, but progress has been stubbornly slow. The World Health Organization (WHO) estimates that more than 300,000 women die each year from complications in pregnancy and childbirth, while 2.5 million babies die within the first month of life and another 2.6 million are stillborn.
10.7% of maternal deaths and 23% of newborn deaths are due to infections contracted during birth. To reduce this risk, it is essential to ensure the “six cleans”: clean hands, a clean perineum, a clean delivery surface, a clean cord and tying instruments, and a clean cloth for drying. To this end, safe birth kits – packages of sterile materials designed to enhance hygienic practices during delivery– have increasingly been promoted by stakeholders as a promising intervention to enhance maternal and newborn health.

The promise of birth kits is simple: they cost only a few dollars each, are easy to use, and offer the prospect of reduced infection risks for women and babies delivering without medical attention at home, or in facilities that lack the capacity to sterilize equipment. There is some variation in what safe birth kits contain in different contexts, but generally they include a plastic sheet, soap, sterile liquid, a razor blade, cotton wool, gloves, and string.
Despite the recommendations supporting birth kit use, however, there is limited evidence around their effectiveness, especially when kits are used outside the formal health system or during home births. New research presenting a secondary analysis of data from a cluster randomized controlled trial in northern Nigeria – a region characterized by one of the world’s worst maternal mortality rates – suggests that the distribution of safe birth kits to women in their homes was not associated with enhanced health outcomes for mothers or infants.
In this study, birth kits were distributed by community health workers (CHWs) directly to pregnant women in their homes in 72 communities in Jigawa state, and health outcomes were tracked for a period of three years. Jigawa is characterized by generally low rates of maternal health services utilization and poor baseline health outcomes, including the third lowest rate of facility-based delivery among Nigerian states (6.7% vs 35.5% nationally), and the fourth lowest percentage of fully vaccinated children 12-23 months of age (4% vs 25% nationally). In addition, only 11% of women in Jigawa are literate. In this context, the birth kits intervention seemed to be a promising strategy to enhance maternal and neonatal health among a large number of women delivering at home with limited access to skilled health care.
Data was analyzed from 3,317 births observed during this period; 140 women received birth kits, and 72 women used the kits. In general, women who chose to utilize kits were healthier and reported a lower probability of past pregnancy complications than those who did not use the kits. Nonetheless, kit users were less likely to complete four or more antenatal care visits, and were more likely to report prolonged labor and post-partum bleeding than non-users. There was no association between kit use and facility-based delivery or postnatal care. The findings suggest that the use of birth kits did not enhance maternal or infant health, and may in fact have been associated with detrimental health outcomes.

 Ultimately, birth kits alone may be insufficient to generate improved health outcomes for women and newborns, particularly if they are distributed in a low-resource, low-knowledge setting with limited links to the formal health system. While the promise of safe birth kits is a low-cost fix to a persistent health challenge, real fixes may be more complex — and more expensive. This new evidence highlights the crucial importance of identifying strategies to integrate the use of safe delivery kits with other forms of delivery care delivered by trained health workers.
Ultimately, birth kits alone may be insufficient to generate improved health outcomes for women and newborns, particularly if they are distributed in a low-resource, low-knowledge setting with limited links to the formal health system. While the promise of safe birth kits is a low-cost fix to a persistent health challenge, real fixes may be more complex — and more expensive. This new evidence highlights the crucial importance of identifying strategies to integrate the use of safe delivery kits with other forms of delivery care delivered by trained health workers.
Read more about this analysis here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0208885