How results from a multi-country study encourage a review of current global policy and practice to save lives
A blog by Golam Mothabbir, Senior Advisor, Health and Nutrition, Save the Children International – Bangladesh Country Office, and Eric Swedberg, Managing Director, Child Health, Department of Global Health, Save the Children, USA. Photo credits: Save the Children.
In December 2017, 14-month-old Kawser had been suffering from a cold, cough, and fever. His mother, Amena, gave him some medicine following the advice of Kabiraj, the traditional herbal healer of their village in Barishal District in Bangladesh. Unfortunately, Kawser’s condition deteriorated. Tanjila, a community health volunteer, visited the family as a part of her household visit plan. She found that Kawser was suffering from a severe respiratory illness, and counseled his mother that he might have pneumonia and she should take him to Babarkhana Community Clinic. Amena was hesitant due to the high cost of treatments at health centers and her prior experience with her 6-month-old son, Badsha, who died from pneumonia following treatment at both a health facility and hospital for 17 days. Tanjila reassured Amena and said, “You can rely on the community clinic because the service provider is trained on pneumonia management and your son is in the early stage of the disease.”

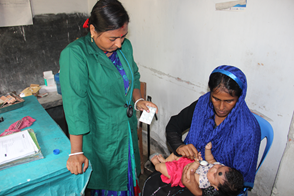
After conversations with her husband, Karim, Amena took Kawser to Babarkhana Community Clinic. The trained community health care provider (CHCP) examined Kawser, counted the respiratory rate with a respiratory timer, measured oxygen saturation with a pulse oximeter, and diagnosed pneumonia without any danger signs. The CHCP gave a first dose of amoxicillin 250mg dispersible tablet to treat Kawser and provided an additional five-day supply to his mother, explaining how to give the medication to her son. She also asked her to come back to the clinic for a follow-up visit. Amena completed the full course of antibiotics following the advice of the CHCP and Kawser was fully cured. She thanked the volunteer Tanjila and the CHCP saying, “I am forever grateful to these two people.”
This story illustrates how timely and appropriate treatment of pneumonia at the community level can save the lives of sick children who may never reach a higher-level facility.
Progress is urgently needed to end preventable deaths among children younger than five years of age
Fifty-four countries are currently off track to meeting Sustainable Development Goal (SDG) 3 child mortality targets. As a result, global health researchers seek to identify and test innovative approaches to increase access to appropriate treatment to those vulnerable children, like Kawser, who are currently not being reached by the health system in their countries.
Pneumonia is the number one infectious killer of children 1-59 months old globally, with over 800,000 pneumonia-related deaths every year. Both integrated management of childhood illness (IMCI) and integrated community case management (iCCM) enable health workers to identify and treat pneumonia. Whereas chest-indrawing (severe) pneumonia cases can be treated effectively according to the IMCI protocols at health facilities, those cases identified by community level health workers (CLHWs) must be referred to the nearest facility. Until recently, there was insufficient evidence on the safety and efficacy of treatment at the community level. Unfortunately, we know that many of these sick children do not access referral care due to the distance to health facilities and cost to families.
Implementing safe and effective treatment of chest-indrawing pneumonia at the community level
A January 2022 multi-county trial in rural areas of four countries (Bangladesh, Ethiopia, India, and Malawi) from September 2016 to December 2018 found that CLHWs can safely treat non-hypoxaemic children 2-59 months old with chest-indrawing pneumonia with oral amoxicillin. In addition to identifying children with hypoxaemia, the study found that the CLHWs correctly performed pulse oximetry in 91.1% of cases.
This new evidence must be used to review the current WHO/UNICEF iCCM protocol and implement these policy changes at the country level. Follow-on effectiveness studies, which are currently proceeding, will also provide important evidence to inform the scale-up of the enhanced management strategies.
These policy and program innovations will lead to increased access to treatment of chest-indrawing pneumonia in children 2-59 months old by CLHWs, particularly in settings where access to higher-level health facilities is limited and referral is not feasible.
One comment