By Karen Walker and Carole Kenner
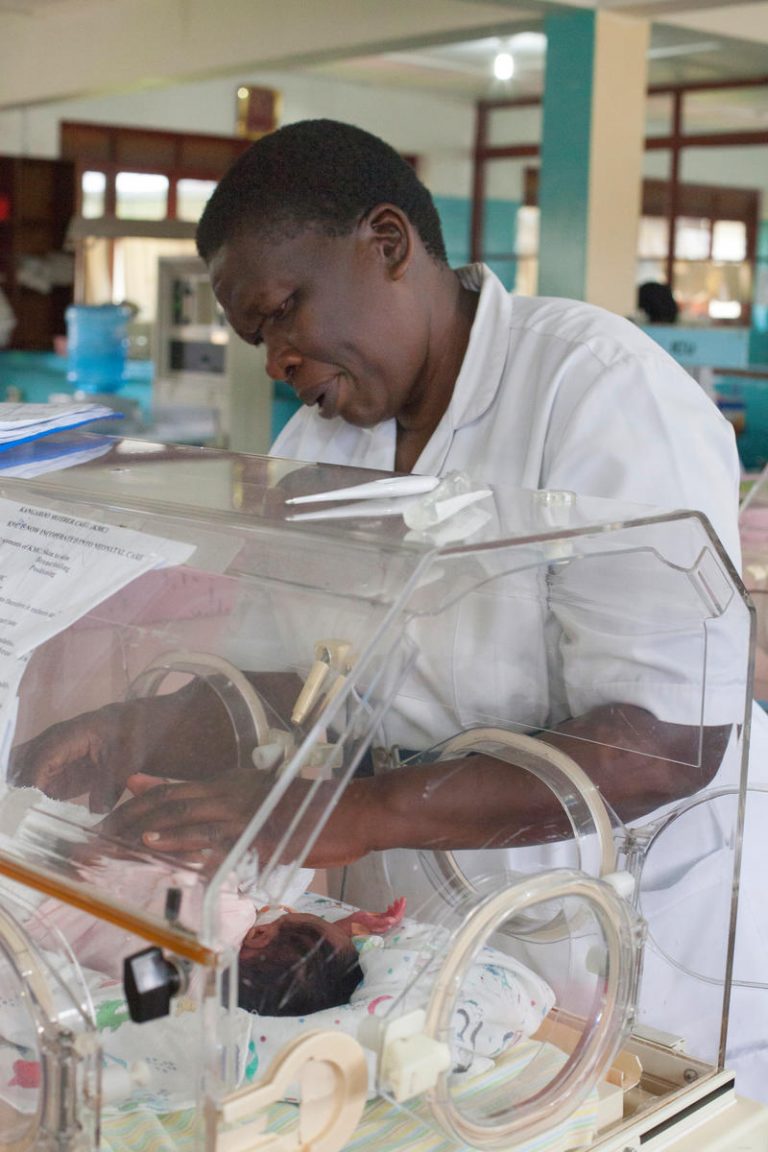
Envisage this – you are a neonatal nurse and you go to work in a busy neonatal unit. Today, however, you are not in your own neonatal unit in your high-income country with ratios of approximately 1 nurse to 1 or 2 babies in intensive care and 1 to 4 in special care. Instead, you are in a low- or middle-income country, where they kindly place you in the “well baby” room in special care. These babies are nearly ready to go home. Here you find yourself the only nurse in that room for that shift – caring for all 45 babies sharing 30 cots as there are not enough cots for all the babies. Four of the babies are sharing phototherapy lights. You are advised that mothers will generally come every three hours to feed the babies, except for the few babies that have no family. Although highly skilled, from a simple mathematics calculation, you realise you have a maximum of 10 minutes to spend with each baby in an 8 hour shift – not including any breaks, writing notes, or new admissions. Reflect a little on how this would affect the quality of your care.
Unfortunately, this is a common scenario in many hospitals, although it is well known that when there are high nurse to neonate staffing ratios, there are increased episodes of missed care, patient safety issues, and poor quality care. [1]
We have an immense challenge ahead of us and we need to address it now. It is predicted that there will be a shortage of 18 million health care workers in the next ten years, and nurses make up nearly half of the health care workforce.[2] However, despite this worrying prediction for the future, we actually already have a crisis – but it is sadly invisible. These impossibly high ratios lead to staff stress and burnout, which not only cause nurses to leave the profession, but it also discourages others from becoming nurses.
It certainly contributes to neonatal morbidity and mortality, and although this scenario describes a special care unit, neonatal intensive care staffing ratios are also dangerously high in many units. To assist countries to achieve the Sustainable Development Goals (SDGs), and decrease neonatal mortality and morbidity we must take action.
What should we do?
Do we need to train more nurses? This seems a logical solution, however it needs to be country specific as new graduate nurses cannot find work in some countries despite having a bachelor’s degree.
Should we just employ more nurses with neonatal knowledge where there are shortages? Definitely, but this needs financial support, as well as hospital and health systems changes. We must strengthen healthcare systems within countries, collecting workforce data to determine staffing ratios, neonatal outcomes, and supply and demand in order to have a well-educated workforce in the most needed areas.
Should we consider task shifting? Again, this is a sensible concept, which definitely needs to be applied at a hospital or unit. When the tasks of qualified neonatal nurses include cleaning equipment, going to the pharmacy and washing floors, there is great scope for task shifting. Again, this needs a financial and systems plan.
A Minister of Health from a fragile region with high maternal and neonatal mortality said recently when we were discussing this issue: “I have a limited budget to spend on health, health of everyone – I need a good financial argument about why I should spend the money here.”
This makes sense, as the money available for health is finite and we must put forward a clear economic argument, which is feasible as there is evidence available on the economic assessment of neonatal intensive care units, demonstrating cost effectiveness.[3]
The argument to provide quality care to reduce not only mortality but also morbidity, which is only possible with sufficient skilled nurses, is strong. We argue that these babies are the future workforce of each country and therefore the foundation of a stable economy. We also argue that nurses are the backbone of the healthcare system and, as such, are an economic driver. Changes to support a country’s achievement of the SDGs to decrease neonatal mortality and morbidity are not just the right thing to do: they are economically critical to a country’s growth.
Now is the time for a “call for action,” and for all national and global health care worker organizations and families to add their voices. Access to quality health care is a human right for our neonates and we need to advocate for this right!
[1] Cooley HL, Mara CA, Carle AC, Mark BA, Pickler RH. Association of nurse workload with missed nursing care in the Neonatal Intensive Care Unit. JAMA pediatrics. 2019 Jan 1;173(1):44-51.
[3] Cheah IG. Economic assessment of neonatal intensive care. Translational Pediatrics. 2019 Jul;8(3):246.