A post from the Stillbirth Advocacy Working Group stillbirths series by Dr. Linda Vanotoo
The voice of the stillborn is too silent to be heard. Ghana is committed to improving the health of pregnant women and newborns. There are a lot of social pro-poor interventions going on in Ghana to ensure that pregnant women have access to skilled care during pregnancy and delivery. Under the National Health Insurance Scheme, pregnant women can access services including antenatal care and delivery and the babies have access to free care for the first three months linked to their mothers after which period the child is registered as an individual.
Newborn deaths contribute significantly to childhood deaths in Ghana. As a means of reducing newborn deaths in Ghana, the 2014-2018 Newborn Strategy and Action Plan (NBSAP) was specifically developed for implementation. The development of the document is a laudable idea, however most of the attention is on live births and there is very little mention of stillbirth and very few interventions developed specifically for reduction of stillbirths. According to the Ghana Health Service, 2016 Annual Report (page 92), stillbirth forms about 1.7% of total deliveries in Ghana annually.
 The Hope Restoration Centre provides an opportunity for mothers and families who had stillbirths; lost their babies or had complicated birth outcomes to receive psychosocial support; have their questions answered and help through the grieving period.
The Hope Restoration Centre provides an opportunity for mothers and families who had stillbirths; lost their babies or had complicated birth outcomes to receive psychosocial support; have their questions answered and help through the grieving period.
The response to delivery of a stillbirth is dependent on the cultural belief and practices of the affected family. There are many tribes in Ghana, but generally stillbirth is one subject that is hardly discussed openly at home or within the health sector. In the home, the affected mother is encouraged to grieve for a short period and at the hospital level, the health worker encourages the mother to get herself together as quickly as possible and plan for the next pregnancy (read more here). There are good intentions behind these responses – for the mother to focus on a brighter future and delivery of live birth in a subsequent pregnancy. The needs of the families are not met as they continue to ask questions but never get answers. “The cry is too silent to be heard by the health sector.”
In my opinion, one of the ways to facilitate discussion around stillbirth openly and more often is to place it on a national agenda. This is why the development of the new NBSAP is seen as a good opportunity to give a voice to “the silent cry of stillborn babies and their families in Ghana for more attention.” To get stillbirth onto the national agenda, I designed a stillbirth audit form, which I administered to nurses to use to audit stillbirth. The results were accepted for a poster presentation at the first fetal growth conference in Birmingham, UK. This served as one of the reference documents for the development of a national perinatal audit tool for Ghana. I served as a member of the Steering Committee that developed the NBSAP and advocated for more focus on stillbirth. In my opinion, a lot has been achieved. As a result, in collaboration with other advocates, stillbirth has been given more space in the current 2019 – 2024 NBSAP (publication forthcoming).
 The Annual Promise Conference – Stillbirth is always discussed.
The Annual Promise Conference – Stillbirth is always discussed.
Getting stillbirth on the national agenda is not seen as pushing away other important issues; however, it is a way of saying that there is need to give stillborns the same attention that is given to babies born alive and high quality respectful care to women and babies (whether live or stillborn). In this regard, women whose pregnancies end as stillborn should receive post loss care, which is virtually nonexistent. I have invited women who have had stillbirths to share their stories during meetings on maternal and newborn health and the following is a quote from a mother: “… I have had 2 stillbirths but no one explained why they happened to me; I have therefore decided not to have more children…” Another woman expressed her deep pain and sorrow at the loss of her baby at birth, saying, “I don’t want to see my baby dead.”
This is the time to act. Paediatricians, policy makers, development partners, midwives and nurses were involved in the drafting of the NBSAP and contributed to inclusion of issues on stillbirth. Although there is an improvement in the attention given to stillbirths, more needs to be done to involve affected families and provide post loss care for the mothers and their families.
This post from a member of the Stillbirth Advocacy Working Group (SAWG) reflects the perspective of the author alone; it does not represent the views of the SAWG.
The Stillbirth Advocacy Working Group was founded by the Partnership for Maternal, Newborn and Child Health, and is co-chaired by the International Stillbirth Alliance and the London School of Hygiene & Tropical Medicine. Email co-chairs Hannah Blencowe or Susannah Leisher at hannah-jayne.blencowe@lshtm.ac.uk or shleisher@aol.com to learn more, or sign up to join the group here!
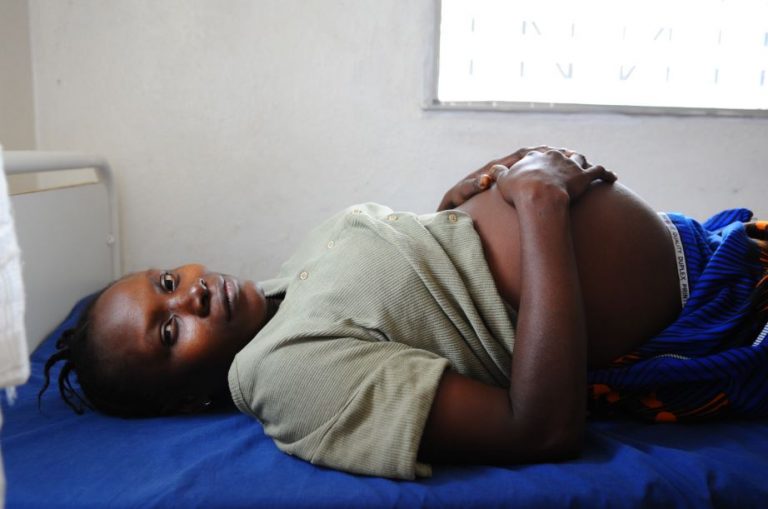
 The Annual Promise Conference – Stillbirth is always discussed.
The Annual Promise Conference – Stillbirth is always discussed.