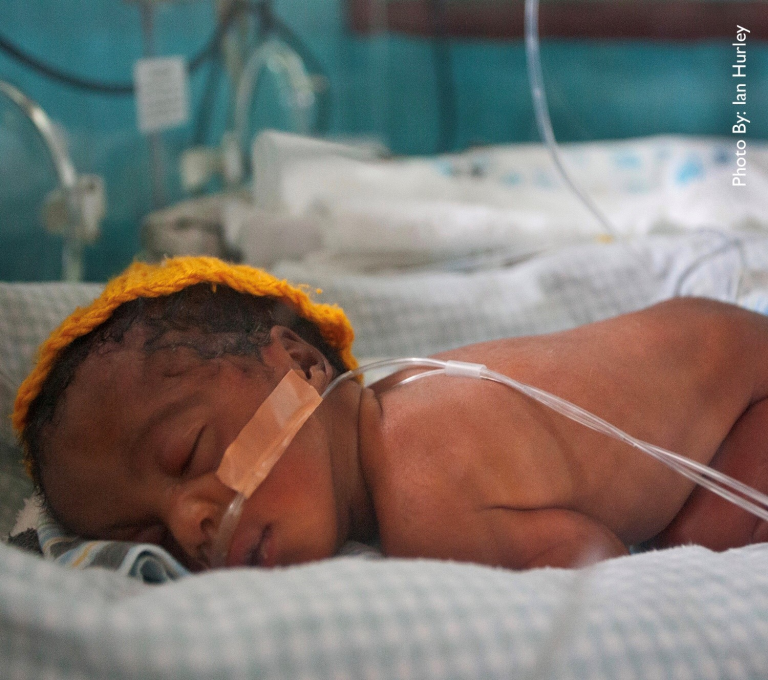
The following typical anecdote served as the urgent impetus to develop a strategy to reduce premature infant mortality in Tanzania, a low resource country. Rounding in a newborn intensive care area where babies are not routinely monitored (see Picture 1), the care team came upon a 30 week premature infant who had been born vaginally with Apgar scores of 9 and 9 at one and five minutes. The infant had been stable during the first 24 hours following birth, and was being cared for in an open bassinette. The infant was now noted to be breathing very rapidly and the rib muscles were pulling in. The caring physician reviewed the perinatal history which was unremarkable and started antibiotics. However the infant’s condition rapidly deteriorated and died within 12 hours.
 Picture 1: Courtesy of Dr Augustine Massawe
Picture 1: Courtesy of Dr Augustine Massawe
There are approximately 9500 premature infants who die annually in Tanzania which equates to approximately one per hour. The major causes of death include birth asphyxia (inability to establish spontaneous respirations at birth), breathing problems related to the premature lungs, infection (which often cannot be predicted from the history) and complications from a low body temperature at birth. In Tanzania there is limited ability to support the babies breathing if indicated, with anything more than providing oxygen.
To address this critical problem we focused on premature infants at 28 to 34 6/7 weeks estimated gestational age via the pilot implementation of a Premature Care Bundle. The bundle was tested at four Tanzanian hospitals between July 2015 and June 2017 and included: administration of antenatal corticosteroids to mothers in preterm labor to facilitate lung maturation, administration of antibiotics to mothers when in active labor, immediate stabilization/resuscitation of the newborn (to facilitate the onset of spontaneous breathing), avoidance of a drop in body temperature < 36 OC (moderate hypothermia), and administration of early neonatal antibiotics. The care bundle reflects standard interventions undertaken in the USA on a daily basis. The care bundle costs less than $7 per medication for both mother and baby. That’s about the cost of a large latté at Starbucks.
A core group of investigators which included Obstetricians, Midwives and Pediatrics, representing three university-affiliated hospitals and one district, facilitated implementation of the care bundle. The pre- versus post-implementation findings of the study, which were recently in the March 2018 issue of PlosOne, saw an overall 26 percent reduction in neonatal mortality from 166/1,000 to 122/1,000 live births, and a 33 percent reduction in fresh stillbirths from 162/1,000 to 111/1,000. (Picture 2) By subgroup analysis, for premature babies, 28 to 30 6/7 weeks, there was no reduction in mortality. However, for the “larger babies,” i.e. 31 to 34 6/7 weeks, there was a 45 percent reduction in deaths. The most striking success was achieved when the care bundle included a combination of medications, for example, steroids and neonatal antibiotics versus none – a 70 percent reduction in mortality was achieved.
This care bundle serves as a bridge between events during labor and the first postnatal “Golden Hour”- a time period where the midwife is invariably the sole provider. Thus, a major emphasis was placed on empowering the midwife with a knowledge that provided the rational for the intervention strategies. After an hour, the infant moves from the delivery area to a neonatal area where other programs such as Essential Newborn Care and Saving Newborn Lives are implemented.
The findings of our study are consistent with proof of concept, and the positive outcomes in part reflect the commitment of the care providers, who believed in this low cost strategy. If these findings can be replicated in other resource-limited settings, the ability to further reduce the less than five-year mortality rates becomes enormous.”
 Picture 2: Reducing preterm infant mortality in Tanzania care bundle implementation outcomes
Picture 2: Reducing preterm infant mortality in Tanzania care bundle implementation outcomes