It is anticipated that that COVID-19 (the disease caused by the novel coronavirus named SAR-CoV-2) will occur in most, if not all countries.
A key fact about COVID-19 is that the vast majority of infections will result in very mild or no symptoms. Not everybody is at risk of severe disease. Persons of advancing age and those with existing respiratory, cardiac and/or metabolic disorders and immunodeficiencies are at higher risk of moderate to severe disease.
Limited data are available on COVID-19 in pregnancy, but the studies published to date do not show an increased risk of severe disease in late pregnancy or substantial risk to the newborn. Congenital infection has not been found, and the virus has not been detected in expelled products of conception. These findings are reassuring, and are quite different from other recent pandemics, like the 2009 H1N1 influenza A pandemic which resulted in more severe disease in pregnant women, or Zika virus which is teratogenic. Information on the impact of COVID-19 on early pregnancy outcomes remains unavailable at the time of writing. Non-pregnant women of childbearing age are also at low risk of severe disease.
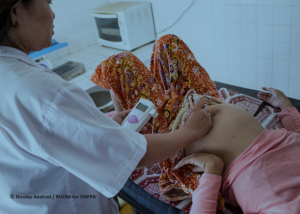
The impact on acute care services in settings with under-resourced health systems is likely to be substantial. Maternity services should continue to be prioritized as an essential core health service, and other sexual and reproductive health care such as family planning, emergency contraception, treatment of sexually transmitted diseases, post-abortion care and where legal, safe abortion services to the full extent of the law, also need to remain available as core health services.
Maternity care providers (including midwives and all other health care workers providing maternal and newborn care), whether based in health facilities or within the community, are essential health care workers and must be protected and prioritized to continue providing care to childbearing women and their babies.