Quality and infrastructure upgrades improve maternal and child health in Sierra Leone
This blog was originally published by USAID MOMENTUM Country and Global Leadership program.
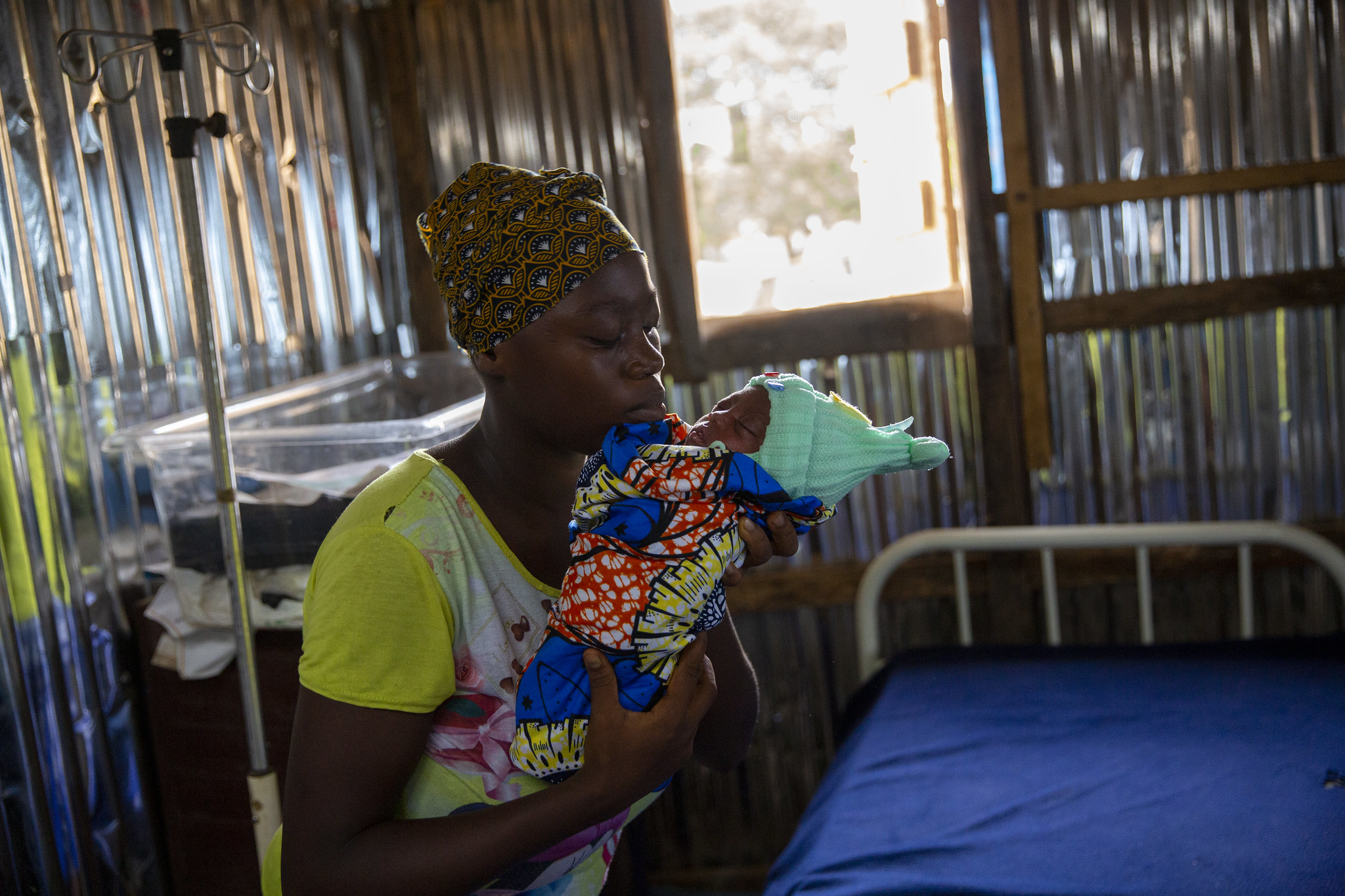
The day after giving birth to a healthy baby, Fatima and her newborn returned to the Maternal and Child Health Post in Thompson Bay, an under-resourced community in Freetown, Sierra Leone, for a routine checkup. At the clinic, community health nurse Rebecca Swaray, who helped deliver Fatima’s baby the day before, checked in on the new mom and her firstborn.
This was Rebecca’s dream and vision come to life: providing a space where expecting parents, new mothers, and newborns could get the care they need.
During the rainy season in 2017, Rebecca used her own personal funds to help build the one and only health clinic in Thompson Bay, a semi-permanent structure made of zinc sheets.
“I could not stand the sight of children, mothers, and pregnant women drenched by rain while waiting for medical checkup and treatment.” – Rebecca
The clinic serves a population of 11,000 people, including residents of other informal settlements around Thompson Bay. On average 300 patients visit the clinic every month, over half of those being children under 5.
“I did not do this because I am rich,” Rebecca says. “I am like any average nurse. I did it because I felt I should help the Thompson Bay community, especially because I knew this would benefit the children and the pregnant women.”
MAKEOVER, HEALTH POST EDITION
 Rebecca’s makeshift health post was among the first of 53 facilities selected by Sierra Leone’s Western Area Urban District Health Management Team and USAID’s MOMENTUM Country and Global Leadership project to implement water, sanitation, and hygiene (WASH), infection prevention and control standards, and structural improvements amid the pandemic.
Rebecca’s makeshift health post was among the first of 53 facilities selected by Sierra Leone’s Western Area Urban District Health Management Team and USAID’s MOMENTUM Country and Global Leadership project to implement water, sanitation, and hygiene (WASH), infection prevention and control standards, and structural improvements amid the pandemic.
The transformation of the clinic in 2021 created a safer structure, with sturdier doors, mesh windows, and shutters to keep the bugs and rain out. Improvements also included procurement of updated equipment and WASH materials like soap, disinfectant, a handwashing station and personal protective equipment. One of the most exciting additions was a new delivery bed. Before, the facility had only one and it was difficult to clean and disinfect in between deliveries.
“At first most clients didn’t come to the facility because of the condition of the facility …,” Rebecca explained. “As a result of the innovation from MOMENTUM, the condition is much better, and we are also supported with infection prevention and control materials (soap, gloves, handwashing) so that more clients are coming.”
A GREAT NEED FOR MATERNAL HEALTH INVESTMENTS
Sierra Leone has the third-highest maternal mortality rate in the world. In West and Central Africa, only 60 percent of women give birth in a health facility. Women opt to deliver at home due to poor quality services and infrastructure—including limited beds, no running water, and no electricity.
Sierra Leoneans have experience with infectious diseases. Many lived through the Ebola epidemic in 2014 and 2015 and came to associate health facilities with poor outcomes. Fears surrounding the COVID-19 pandemic further threatened care-seeking access to health service.
Weather also impacts where a pregnant person decides to give birth, as Rebecca noticed. Heavy rains and a leaking roof in the labor and delivery room led staff to refer women in labor to facilities much further away. In some cases, patients opted to deliver at home rather than travel to the community facility. Rebecca hopes the remodel will provide a safer and more comfortable space to provide care during pregnancy, labor, and delivery, and for new mothers.
“It’s important [for mothers to deliver at the clinic] so that I can monitor the development of the baby and check on the condition of the mother,” said Rebecca. “Also so that I detect any danger signs, so that I can take quick action.”
Midwife Hannah Kanneh, who has worked alongside Rebecca for seven years, educates mothers like Fatima on health, nutrition, and infectious disease prevention during pre- and postnatal care sessions.
At Fatima’s visit, she talked about the importance of exclusive breastfeeding for the first six months of the child’s life, and advised Fatima against giving the baby water.
Hannah also instructed Fatima to bring the baby back to the clinic if he gets a fever, and to avoid feeding the child with her hands in order to prevent spreading germs. Fatima will continue to visit the clinic for vaccines, and to weigh her son each month until he is 6 months old.
See more photos in the original post here.
